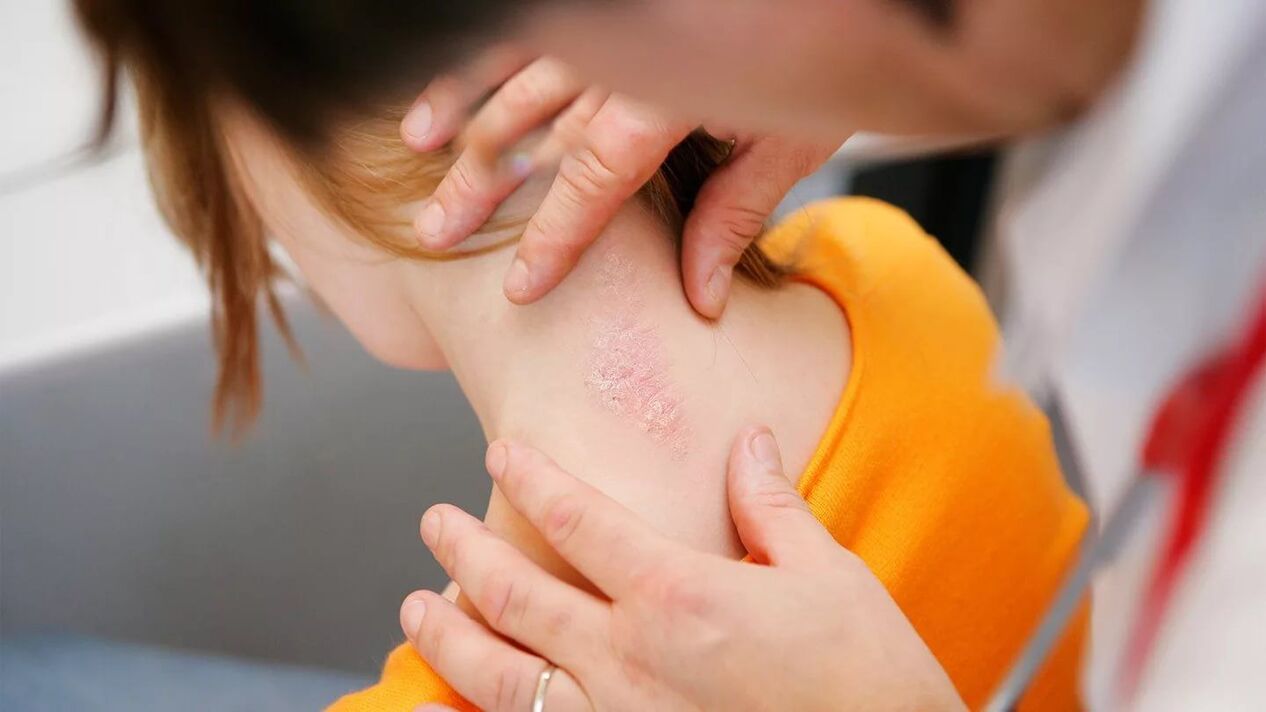
causes of psoriasis
- Stress, negative emotional experience;
- endocrine pathology;
- genetic predisposition;
- A malfunction of the immune system leads to disruption of the growth and division processes of epithelial cells.
- The skin is very thin and poorly hydrated (produces little sebum).
- Frequent exposure to irritating compounds – low-quality cosmetics, alcohol solutions, household chemicals.
- Wash your body and hands frequently (especially with a stiff towel and antibacterial soap/body wash).
- Alcohol abuse.
- Development of infectious diseases caused by staphylococci, streptococci, fungi.
- Take antidepressants, lithium carbonate, beta-blockers, antimalarials, and anticonvulsants.
- Changes in climate zones.
- Mechanical damage to the skin.
- Predisposition to allergic reactions.
- HIV infection.
Disease classification
- Scalp psoriasis (which manifests as itching, cracking, and bleeding of the skin).
- Nail psoriasis (where the nail plate gradually separates from the nail bed and becomes painful, with red spots forming on it).
- Palmoplantar psoriasis (this disease is common only on the soles of the feet and/or palms).
- Skin psoriasis (dry patches on different parts of the body).
- Arthropathic psoriasis (joints are affected).
- Genital psoriasis (a disease affecting the skin of the reproductive organs).
- Common or vulgar. It looks like small, flat, pink pimples that are slightly higher than healthy skin. The tops of the pimples are covered with light scales, and the scales begin to fall off even when touched lightly. If psoriasis treatment is not started promptly, small lesions can coalesce into large lesions.
- Exudative. It is more common in people with obesity, hypothyroidism, and diabetes. Symptoms of this form of psoriasis are as follows: The papules are bright red in color with yellowish-gray scales visible on their tops. Plaques can affect skin folds—the armpits, the area beneath a woman's breasts. The patient complained of itching and burning sensation.
- Seborrheic. Psoriasis is found on the head, behind the ears, in and around the nasolabial folds, between the shoulder blades, and on the chest. The borders of the spots are not well defined. The peel is silvery yellow. If you see a picture of psoriasis on your head, you'll associate it with common fungal diseases like dandruff.
- Palm soles. The disease tends to occur in people aged 30 to 50 who are engaged in heavy manual labor. With this form, a rash may also appear on the body.
- Pustules. Pustules form on the body. Medically, another type of pustules is found - Tsumbusch psoriasis. It may be idiopathic (primary) - blisters appear on the skin that turn into pustules. The pustules open and dry. Later, a scaly rash typical of the disease appears on the body. It is also a secondary benign course. In this case, pustules appear on the surface of typical psoriatic plaques due to the irritating effects of the medication.
Another type of pustular psoriasis is Barber's psoriasis. It only affects the soles of the feet and palms of the hands. Purulent pustules may be seen on the skin. They won't open and over time they turn into a dark, dry crust. Babett's psoriasis is characterized by the symmetry of the lesions. - Arthropathy (arthrosis). Serious form. Occurs in patients with rash. If psoriasis is not adequately treated, it usually occurs five to six years after the first symptoms appear. Pathological conditions of the joint system can vary from mild joint pain, which does not lead to changes in the joint apparatus, to deformative ankylosis, in which the joint becomes completely immobile.
- Psoriasis erythroderma. This is the result of vulgaris or exudative psoriasis. Almost all skin types can be affected. It turns red and is covered with numerous dry scales. The body temperature rises and the lymph nodes (especially in the femur and groin) become swollen. If patients don't learn how to treat psoriasis, they may experience hair loss and brittle nails.
- summer;
- winter (most common);
- uncertain.
Symptoms of psoriasis
As for the nail plate, the most common types of damage are:
- The nails are covered with pits that look like puncture marks ("thimble type").
- Nails change color and begin to fall off, similar to a fungal disease. Psoriasis papules with surrounding red edges can be seen through the nail plate.
stages of psoriasis
- Progressive (initial). New growths appear on the surface of the skin as a rash, often growing along the perimeter. They spread into healthy skin and form oval or round patches. The spots are pink or red. They don't have the flaky crust on them yet - just white scales. The edges of the lesion were slightly compacted. A new rash may appear due to scratching.
- fixed. One to four weeks after the first symptoms of psoriasis appear. The plaques become lighter. New rashes will not appear and old rashes will slowly disappear. Papules heal in a direction from the center to the edges, which is why their shape becomes a ring. The entire surface of the healed lesion is covered with flaky white scales.
- Regression (fading). The color of psoriasis plaques is almost indistinguishable from healthy skin. Itching is minimized. A "Voronov collar" forms around the lesion, which is a ring of dense layers of keratinized skin. If the patient uses a good quality psoriasis ointment, the resolution phase will last about a month. Otherwise, the "fading" process can take up to six months.
How is psoriasis diagnosed?
How to treat psoriasis
- general treatment;
- topical treatment;
- physiotherapy.
- Vitamin A derivatives (retinoids). Reduces keratinocyte maturation rate. Normalizes cell differentiation and maturation.
- Immunosuppressants. Reduces the activity of T lymphocytes, thereby promoting epidermal cell division.
- Drugs to treat malignant tumors. Inhibits the reproduction and growth of atypical skin cells.
- Selective phototherapy. Irradiate the affected skin with ultraviolet light of wavelength 280-320 nm. Between 15 and 35 procedures are prescribed.
- Photochemotherapy (PUVA therapy). The method involves the combined use of internal photosensitizers and external long-wave UV irradiation. Ultraviolet rays penetrate deeply into the skin, and the photosensitizer blocks the DNA synthesis process of skin cells and reduces their division speed. Course duration is 20 to 30 procedures.
- Laser Treatment. Use laser radiation of different wavelengths. The laser ensures accelerated plaque resorption and eliminates scarring where the plaque is located.
- Use monochromatic UV radiation. Each lesion is treated in turn with a UV radiation lamp/laser source. Healthy skin is not affected. This method is best if less than 10% of the skin area is affected. The duration of treatment is 15 to 30 sessions.
- Electric sleep. The electrical pulses produce mild effects on the brain that last 20-60 minutes. As a result, the patient calms down, the functions of the central nervous system return to normal, and the psoriatic plaques begin to fade.
Ultrasound therapy. It is a decongestant, antipruritic and analgesic. Accelerate scar absorption. If necessary, it can be combined with phonophoresis. To achieve therapeutic effects, 7 to 14 courses are required. - Magnet therapy (Betatron device). It has general healing effects on the body. Relieves inflammation, reduces itching and burning, and helps eliminate joint pain.
- Treat with bee venom. Bee venom is injected into the body using an electrophoresis or ultrasound machine. It is characterized by anti-inflammatory and anti-inflammatory effects, normalizing metabolic processes.
- High fever. Use pads containing the hot mixture to heat psoriasis-affected tissue to 40 degrees. Treatment can help improve the function of the immune system and reduce the negative effects of the disease on the skin.
- Salicylic acid ointment (softens skin, reduces inflammation, and removes dead skin cells);
- Anthracene (slows down DNA synthesis, reduces the activity of cellular enzymes, and slows down the cell division process);
- Sulfur ointment (disinfects, softens, removes white patches on lesions);
- Naphtadiol ointment (relieves itching, relieves pain, normalizes immune response).
- Hydrocortisone. Eliminates tightness and itchiness. Inhibits the increase in white blood cell activity and prevents them from entering the skin.
- Flumetasone. Helps treat exudative psoriasis. It is characterized by significant anti-allergic, anti-inflammatory and antipruritic effects.
- Triamcinolone acetonide. It has anti-itching and anti-inflammatory effects. Expressed during exacerbation.
- UV comb (promotes keratinocytes to contour skin cells, thus reabsorbing existing plaque).
- Photochemotherapy (UVR combined with Beroxan, Puvalen and Psoralen).
- Medicated shampoos (Tana, Nizoral, Friedem tar). It is recommended to purchase several different products and use them interchangeably. This avoids addiction.
- Salicylic acid ointment (apply to the separated area, cover the head with cellophane and leave for two hours).
- Hormone lotions (Belosalik, Elokom, Diprosalik). Contains steroid hormones. Easily applied to the scalp to effectively eliminate flaking and itching.
- Kirkazon decoction (normalizes skin cell division process, cleanses).
- Herbal teas made from dandelion root, St. John's wort, or nettle leaves.
- Add rope, soapweed, or yarrow decoction to the healing bath.
- Rub the affected area with cabbage brine, celandine juice, and birch tar.
Compression based on garlic infusion.
psoriasis diet
- Fruit (apples, apricots, peaches);
- fruit juice;
- Vegetables (beets, potatoes, radishes, watermelon, pumpkin);
- greening;
- Berries (all berries except red berries);
- Lean meat (beef, veal, turkey, rabbit) – up to 200 g per day;
- any nuts;
- lean fish;
- cultured dairy products, cottage cheese and cheese;
- Whole wheat bread;
- Sea kale.
- smoked dishes;
- red fish;
- animal fats;
- Egg;
- pork and duck;
- Baked goods.
Is psoriasis dangerous?
risk groups
- chronic skin diseases;
- skin damage;
- Disorders of the central nervous system and autonomic nervous system.
prevention
- Moisturizes skin;
- Avoid staying in cold, dry rooms for long periods of time;
- Avoid taking beta blockers and lithium (except in extreme cases) as they can trigger psoriasis.























