Psoriasis, or psoriasis, is a chronic autoimmune disease that affects the skin and manifests in the form of erythematous plaques covered with small scales. There is no cure for the disease, so treatment for psoriasis reduces to managing symptoms, stopping pain and inflammation, and achieving early and long-term remission. There is a lot of prejudice against this disease in society. People who don't know what think psoriasis is contagious. In the description, several types of this NCD can be distinguished, each with its own symptoms and course.
Where does psoriasis come from
The cause of psoriasis has not been determined, as little is known about this skin condition. Symptoms in the early stages of the disease may resemble dermatitis and eczema, but it is impossible to confuse overt psoriatic plaques with other skin conditions. Scientists and doctors agree that one of the factors in the emergence of psoriasis is a genetic predisposition.
For example, if a mother is diagnosed with a skin disorder, the child has a 15 percent chance of inheriting the disorder. If both parents are treated for psoriasis, the risk of genetic transmission of the disease increases fourfold, to 60%.
But even if a parent is a carrier of the gene that causes the skin disease, that doesn't mean the child will get sick. The causes of psoriasis on the body are different. Stress, nerve shocks, mental trauma "trigger" skin diseases.
Psoriasis is also due to:
- skin lesions, burns, insect bites, tattoos;
- the medicine the person is taking;
- infectious diseases;
- alcoholism, smoking;
- exposure to chemicals, such as detergents;
- Dermatitis and fungal diseases;
- HIV;
- Pregnancy and childbirth.
Recently, scientists have suggested that psoriasis may arise due to malnutrition, but no convincing evidence has been found to support this theory.
Doctors know a certain gene is responsible for the skin disease, but they can't pinpoint the exact cause of psoriasis.
What does psoriasis look like in its early stages?
The first symptoms of psoriasis are as follows:
- A person's nails fall off and the skin cracks.
- Pustules appear on the body.
- The skin begins to peel off and die.
- Blisters on hands and soles.
- Itchy red spots covered with white scales on elbows, knees, face.
A person falls into depression, is not interested in anything, notices a breakdown or even low self-esteem.
Head, face and under hair
First, a person notices increased skin flaking, similar to dandruff. Then the plaque itself appeared, covered with silvery scales. The rash grows, affecting the increase in skin area, but even with overt psoriasis, the hair does not fall out.
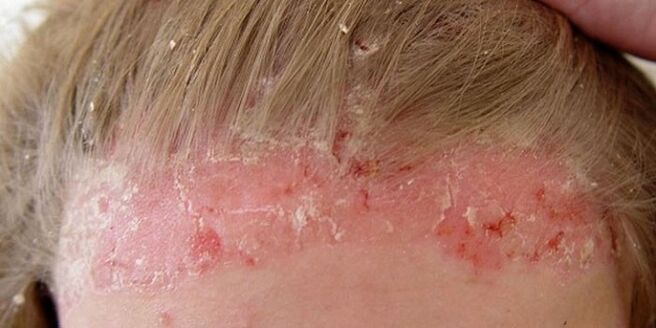
In 80% of cases, psoriasis mainly affects the scalp. If the pathology is not treated, the rash can appear elsewhere.
Severe itching is a harbinger of a disease that affects the skin of the face. At first, psoriasis resembles an allergy, and the skin is covered with small red spots that grow larger and coalesce to form inflamed nodules or papules.
The eruption covers the entire face. The spots themselves are covered with scales that separate easily and painlessly. Beneath them is a terminal film that resembles scarlet glossy leather. If you comb the itchy areas, they will be covered in small droplets of blood.
on arms and legs
The skin disease psoriasis affects the skin:
- upper arms and legs;
- brush;
- knuckles on the hands and feet;
- near the nails.
The disease begins with the appearance of small, round, red areas on the skin between the fingers, calves, wrists, elbows, and knees.
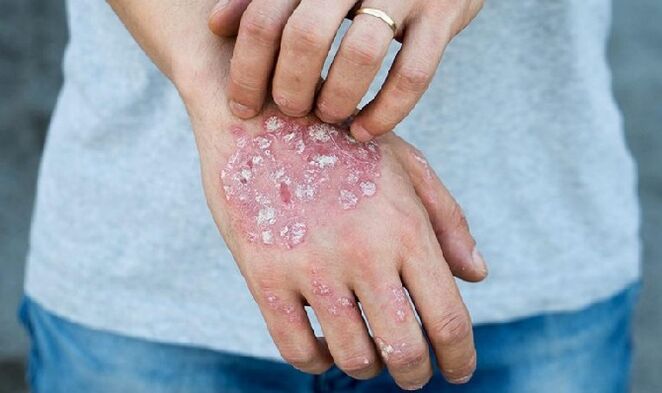
In 10% of cases, psoriasis affects the nails. Psoriasis plaques appear on the nail plate long before the main symptoms of the disease affecting the body's skin.
on palms and feet
Palmoplantar is known as a manifestation of psoriasis, and it affects the skin of the palms and feet.
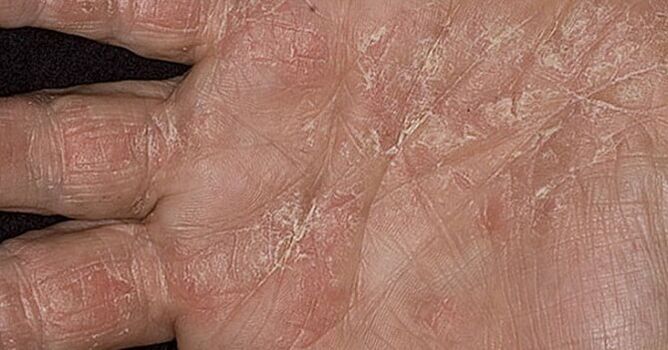
It is characterized by the appearance of red scaly spots covered with white scales. At the site of the rash, the skin thickens, cracks, and becomes inflamed. The form of exacerbation is the formation of pustules, deep abscesses.
on the torso
Signs of a disease that affects the skin of the body are similar to psoriasis on the palms and feet, head, and face. The rash often appears on the back and lower back.
The red spots are covered with gray scales, itchy. They cannot be groomed because the thin end membranes do not protect the smallest capillaries and the skin surface is covered with tiny blood droplets when groomed. Psoriasis can appear on the chest and sides.
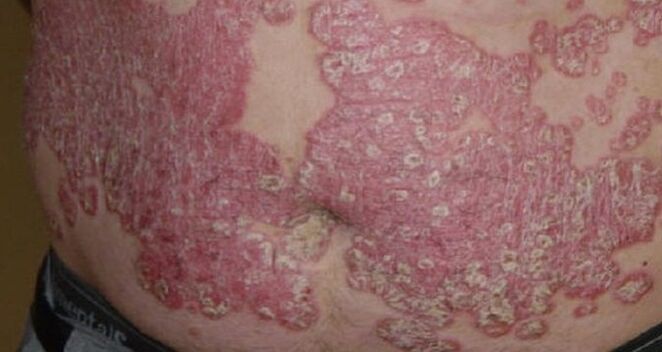
The red dot expands and merges into what doctors call a "paraffin lake. "
Psoriasis can cause various skin changes:
- peeling;
- thickening;
- edema;
- The appearance of blisters and pustules.
Often, keratinized dry skin can crack, which can cause pain and discomfort.
Other localization
If the disease is spreading, psoriasis can spread throughout the body. Psoriatic plaques can be located in the groin, buttocks, elbows, and knee folds. The disease can cause a lot of discomfort because the rashes can be itchy, but they should not be scratched. Careless movements can easily damage the thinned affected skin and lead to additional infections.
The symptoms of cutaneous psoriasis are similar regardless of the location, so dermatologists diagnose the disease by:
- A red rash with a well-defined border;
- The so-called triad of psoriasis: the phenomenon of "stearoid plaques", the plaques themselves, covered with silvery soft scales, with a terminal membrane underneath, and in the case of plaques, covered with tiny droplets of blood. scratch;
- New plaques appear at the site of skin damage;
- itching.
psoriatic arthritis
This complication affects joints and tendons, causing them to lose their density and elasticity.
Arthritis, which accompanies the symptoms of psoriasis, is characterized by inflammation of the joints, divided into:
- Asymmetric, affecting several joints on one side of the body, not paired skeletal elements.
- Symmetrical, similar to rheumatoid. Paired joints suffer. This form often results in disability.
- The distal interphalangeal joint, which affects the phalanges of the fingers and toes.
- Spine, in one or more departments.
- Deformed when the joint is destroyed.
Joint inflammation is characterized by severe pain, swelling, and a bluish tinge of skin over the affected bone and joint. In this condition, a person experiences a breakdown and sometimes an increase in lymph nodes.
Classification of psoriasis
The types of psoriasis vary depending on the nature of the rash. The International Classification describes 10 autoimmune chronic diseases:
- The most common is plaque or simplex psoriasis. It affects any part of the body and occurs in both women and men. It begins as a red, swollen spot, which is then covered with a white, peeling, scaly film called a "plaque. "
- Guttate psoriasis affects the skin after a strep infection. It manifests in the thighs, calves, and also affects the neck and back. A red, blue, lavender rash that rises above the surface of the skin and is shaped like a drop of water.
- The mottled form is characterized by a widespread rash all over the body. The disease is more common in women than in men.
- Pustules are the most severe and can be distinguished by the appearance of blisters - pustules surrounded by red, inflamed skin and filled with clear fluid. If the infection gets into the blisters, fragments of pus can appear in the contents.
- Follicles, which affect the skin of the legs and thighs, appear as small white papules.
- Psoriasis on the surface of the flexor muscles, affecting the skin in folds, such as knee creases, groin, under breasts, armpits.
- Palms and soles, often appearing in people who are engaged in manual labor.
- Psoriatic onychomycosis affects only the fingernails and toenails. Discoloration, yellowing, peeling, and sometimes peeling of the nail plate. The skin around the nails thickens.
- Scalp, characterized by a red, scaly rash in areas of hair growth and itching.
- Seborrheic, most common in the chest, behind the ears, between the shoulder blades, and in the nasolabial fold. Psoriatic lesions are highly flaky, often resembling eczema, and covered with purulent crusts.
- The symptoms of erythrodermic psoriasis are obvious. The affected skin may slough off with the board, and a person may experience severe pain and an increase in body temperature. Untreated erythroderma can flow into pyoderma - a purulent lesion of the skin that can lead to death.
Any form of psoriasis requires prompt treatment and should only be prescribed by a dermatologist after examination and necessary research.
How psoriasis manifests in different stages
There are 4 stages in the development of psoriasis:
- initial or early;
- progress;
- stationary;
- backwards.
In most cases, psoriasis begins with the appearance of small papules. Round pink shiny spots, sometimes no larger than the needle, protruding from the surface of the skin with a well-defined border. They are covered with silver scales. A rash in the early stages of psoriasis can be confused with eczema or an allergic rash.

The clinical manifestations of the disease vary in different stages. For example, severe skin inflammation is characteristic of an acute or progressive form that requires medical attention and intensive treatment.
However, the rashes did not go away, but increased and merged with each other. The psoriatic plaques, visibly limited by the pink corolla, begin to flake off. The affected skin is unbearably itchy.
From 2 weeks to several months, psoriasis goes into a stable phase. The growth of psoriatic plaques stops and the peeling increases, covering the entire affected skin area.
As the psoriasis subsides, the peeling fades away and the psoriatic plaques flatten and fade away. There are no marks, scars or scars on the skin. Hyperpigmentation of the skin sometimes occurs. During the remission phase, the skin acquires normal color and texture.
What is the danger of this disease
The severity of the course depends on the skin condition. If the lesions are not extensive, the person is living a normal life. The rash takes up a large area, and people with inflamed skin experience physical and psychological discomfort. A serious health hazard is a complication of pustular psoriasis if the infection gets into the blisters.
Psoriatic arthritis is also dangerous because some forms of it can destroy joints and cause disability. However, osteoarthritis is rare, in 10% of cases.
Even if the patches on the skin are not noticeable and the person feels normal, it is necessary to be examined by a dermatologist who will make a diagnosis and begin treatment. Prompt medical attention will prevent complications and help achieve stable remission.
Comprehensive treatment of psoriasis
There is no effective way to get rid of psoriasis forever. There are various treatments for skin diseases. Prescribe pills, ointments, and physical therapy to a person. A therapeutic bath is recommended and care is taken to take care of the skin condition to prevent injuries such as scratches, cuts, nicks.
Comprehensive treatment for psoriasis works if a person follows medical prescriptions.
How to treat psoriasis with medication
These are the creams, tablets and injections that the attending physician prescribes to those seeking help. The tablets are taken at the designated time before or after meals, the ointment is applied to the affected area with clean hands, and can be injected at home or in the hospital. These can be products based on plant ingredients, hormones and other chemically active substances.
In the complex treatment of scaly lichens:
- Antihistamines, which are prescribed if a person develops allergies.
- Liver-supporting agent.
- Immunomodulators that promote disease progression.
- Immunosuppressants in the form of injections. They are effective but expensive and have serious side effects. Patients with infections or tumors should not use these drugs.
- Sugar steroids are effective but addictive. Therefore, the duration of treatment with hormonal drugs should not exceed 2 weeks.
If scaly lichens appear easily, your doctor will try to limit yourself to topical medications.
Topical - ointments, sprays
Topical treatments for psoriasis are divided into:
- Hormones that affect the body's autoimmune process.
- Therapeutic drugs, including zinc, naproxen, tar, vitamins. They moisturize cracked skin, soften hardened psoriatic lesions, support skin function and restore damaged coverage.
Use hormonal ointments, lotions, and sprays for the skin during exacerbations. Bioactive substances in the ingredients of the powerful cream:
- reduce itching;
- relieve puffiness;
- constrict blood vessels;
- Reduce pain and fight inflammation.
Apply the product to the affected areas of the skin on the body, face and head. Creams are most often used after the acute phase of psoriasis has passed, and doctors do not recommend using hormonal preparations and vitamin D-containing creams for more than 2 weeks.
Pills and Injections
People interested in how to treat psoriasis can ask a dermatologist about effective pills and injections for complex psoriasis treatments.
- If psoriasis is severe, some medicines are prescribed. For example, if the damaged skin does not heal, a person will receive pills.
- Doctors prescribe B vitamins, folic acid, omega acid, other multivitamins, and lecithin. These drugs aid in recovery, are not addictive, shorten the duration of treatment, and prolong remission.
Comprehensive treatment of scaly lichens is not limited to the intake of special agents and vitamins.

Psoriasis is actually not scary to a person if he follows the rules, uses quality makeup, and maintains the health and condition of his skin.
If there are no contraindications, a person can inject drugs containing immunosuppressants:
- Some medications are given subcutaneously, while others used to treat psoriatic arthritis are given intravenously.
- There are serious contraindications to the injection. They cannot be used by persons under the age of 18, pregnant and breastfeeding, with malignancies and infectious diseases.
Homeopathy
Manufacturers of homeopathic medicines claim that the use of such medicines reduces the risk of relapse and guarantees quick recovery from problems. In addition, funding:
- Supports immunity and health of internal organs.
- They are a source of minerals and vitamins that the body needs.
- Restoring the work of the gut, seeding the digestive tract with beneficial bacteria.
- Helps eliminate toxins.
When choosing a drug, homeopaths take into account the patient's medical history, the stage and nature of the course of the disease, genetics, and psychosomatic factors.
Official medicine has no evidence of the effectiveness of homeopathy for psoriasis.
Physical therapy against skin diseases
In most cases, the affected skin is exposed to different lengths of the UV spectrum or laser. Sometimes before surgery, a person takes psoralen, which increases the sensitivity of skin cells to radiation. Doctors also prescribe cryotherapy when the affected skin is exposed to low temperatures. More recently, ultraviolet blood irradiation has been used to treat psoriasis.

Ultraviolet radiation is one of the simplest forms of physical therapy. At the same time, the effectiveness of the method shows fairly confident results.
The duration of sessions varies, but physical therapy is very effective. This is a quick cure for psoriasis. Programs also give a person activities to live and work to the fullest.
Can psoriasis be cured forever? Folk remedies
Squamous lichens are not treatable. Tablets, ointments, and injections fight the symptoms of the disease and reduce the number of relapses. Folk remedies are no exception. Decoctions, tinctures, and therapeutic baths help with the onset of relief, but do not relieve autoimmune diseases.
Oral drugs
Herb- and plant-based means help stop the symptoms of psoriasis. The safest are chamomile decoction, fresh aloe vera juice, compresses and decoctions of rhizomes and burdock leaves.
In pharmacies, you can buy herbal preparations against scaly lichen. They can be brewed with boiling water, brewed and drunk before or after meals, or you can pour them into water and take a therapeutic bath.
According to traditional medicine, the use of hydrogen peroxide can eliminate the manifestations of psoriasis. Use of drugs:
- in the form of a solution. First, dilute one drop in 3 tablespoons of water and drink on an empty stomach half an hour before meals. Gradually increase the strength of the solution to 10 drops for the same amount of water. Take the medicine every three days.
- Superficially, apply to the affected skin for one hour, moisten a sterile gauze with a solution of 2 teaspoons peroxide and 50 ml of water.
Consult your doctor before using any folk remedy.
Compress and bath
Hot compresses and baths with medicinal herbal decoctions do not cure the disease, but they can relieve the general condition and relieve itching and inflammation. External brewing:
- chamomile;
- succession;
- thyme;
- burdock root;
- oak bark;
- Jump;
- Saints etc.
Bathing for longer than 20 minutes is not recommended.

After bathing, apply moisturizing cream and healing ointment to the skin.
Baths and compresses with herbal decoctions have few contraindications.
Skin Protection and Care
There is no complete cure for psoriasis. But during treatment and during remission, a person must take care of the skin properly:
- Avoid trauma to the skin. Don't scrape, don't scrape. Use protective equipment during physical work or cleaning.
- Wear comfortable clothing made from natural materials.
- Use special dermatological cosmetics.
- Moisturize skin.
- Avoid direct sunlight.
Preventive measures also include dietary and lifestyle changes made by the patient.
Lifestyle and Nutrition Changes
Food is not the cause of psoriasis, however, poor nutrition can weaken the body's defenses and reduce resistance to stressors. Therefore, people with lichen scaly need to monitor their daily life and nutrition.
When asked how to treat psoriasis, doctors list preventive measures:
- Avoid heavy, fried, and greasy foods.
- Active lifestyle, moderate physical activity.
- Sunbathe at night and in the morning.
- Quit smoking and alcoholic beverages.
A person should prioritize healthy meals that are high in nutrients, vitamins and minerals.
What to do if your child is sick
The first thing parents notice when they notice lichen scaly on their child's skin is to seek help from a doctor. Treating the disease in its early stages can reduce the intensity of the rash that causes physical and emotional distress in children.
To teach children to properly care for the skin, adhere to a healthy lifestyle. Socialization is very important for children, so parents should encourage children's desire to play sports, make friends, and join circles. To cope with emotional discomfort, children may need the help of a psychotherapist who will teach them not to react to possible silly remarks from peers or even narrow-minded adults.
Can psoriasis be completely cured?
A person facing an itchy, scaly rash that is causing them physical and psychological inconvenience is trying to find out if the disease is being treated.
Learn all about psoriasis and its treatment from the dermatologist you seek help with. There are associations and support centres where you can also get necessary information, including legal information, such as what benefits a person should get if they are diagnosed with psoriasis.
A complete cure for psoriasis is not possible because the disease is linked to genetic factors and genes are not suitable for medication, procedures, homeopathy and folk remedies.
Modern medicines, ointments, procedures are really effective in fighting the symptoms of the disease and prolonging remission. However, psoriasis recurs regardless of the method used. If a person neglects physical examinations and does not follow simple preventive rules, the disease will recur more frequently.
Can this disease be prevented?
The "three pillars" of skin disease prevention:
- Follow personal hygiene rules.
- Proper nutrition nutrition.
- Say goodbye to bad habits.
For washing, it is best to use only cosmetic dermatological products purchased at a pharmacy. Well, if they contain tar.























